The Mako difference
Scan.
Before surgery, a CT scan of your joint is taken and used to develop a 3D virtual model of your unique joint. This allows your surgeon to evaluate your bone structure, disease severity, joint alignment and even the surrounding bone and tissue.
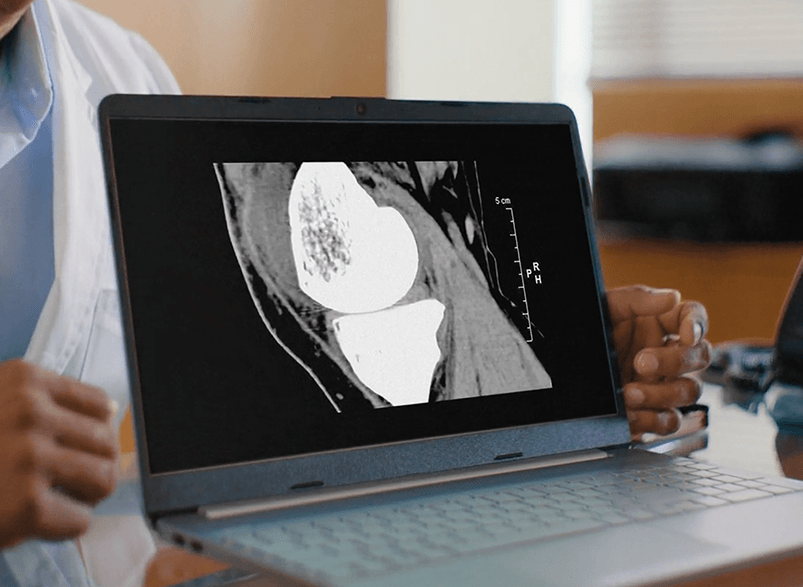
Plan.
Mako’s 3D virtual model of your joint enables your surgeon to create a personalized surgery plan based on your unique anatomy.
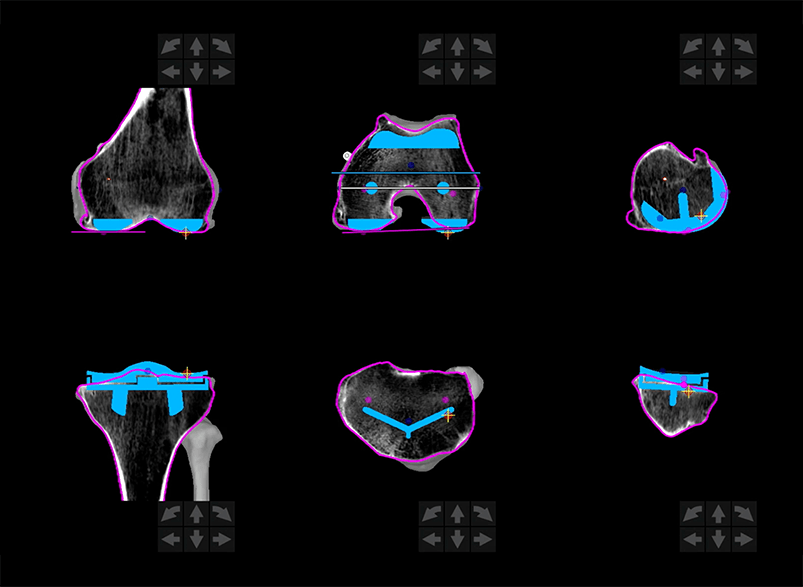
Mako Can.
During surgery, your surgeon guides Mako's robotic arm, which uses AccuStop™ haptic technology, so they can cut less and help protect your healthy bone.1-5
Mako can lead to better outcomes, like less pain and shorter recovery times6-8 compared to traditional joint replacement surgery. Helping to get you back to the things you love, quicker.

Learn more about Mako Robotic-Arm assisted surgery.
Discover Mako SmartRobotics™ surgeons near you to see if a Mako procedure is an option for you.
Explore Mako Robotic-Assisted Surgery
Mako Total Hip Replacement (THA)
Learn how Mako Total Hip can help preserve healthy bone1
EXPLORE MAKO TOTAL HIP
Mako Total Knee Replacement (TKA)
Learn how Mako Total Knee can help protect ligaments9
EXPLORE MAKO TOTAL KNEE
Mako Partial Knee Replacement (PKA)
Learn how Mako Partial Knee has been shown to shorten hospital stay6
EXPLORE MAKO PARTIAL KNEEWatch a webinar now
Find a seminar in your area
References:
- Suarez-Ahedo, C; Gui, C; Martin, T; Chandrasekaran, S; Domb, B. Robotic arm assisted total hip arthoplasty results in smaller acetabular cup size in relation to the femoral head size: A Matched-Pair Controlled Study. Hip Int. 2017; 27 (2): 147-152.
- Haddad, F.S, et al. Iatrogenic Bone and Soft Tissue Trauma in Robotic-Arm Assisted Total Knee Arthroplasty Compared With Conventional Jig-Based Total Knee Arthroplasty: A Prospective Cohort Study and Validation of a New Classification System. J Arthroplasty. 2018 Aug;33(8):2496-2501. Epub 2018 Mar 27.
- Hozack WJ, Chen AF, Khlopas A, et al. Multicenter analysis of outcomes after robotic-arm assisted total knee arthroplasty. Presented at: The Knee Society (TKS) 2018 Members Meeting; September 20-22, 2018; Saint Louis, MO.
- Banks, Scott A, PhD. Haptic Robotics Enable a Systems Approach to Design of a Minimally Invasive Modular Knee Arthroplasty. Am J Orthop. 2009;38(2 suppl):23-27. February 2009.
- Hampp E, Chang TC, Pearle A. Robotic partial knee arthroplasty demonstrated greater bone preservation compared to robotic total knee arthroplasty. Annual Orthopaedic Research Society. Austin, TX. 2-5 Feb 2019.
- Kayani B, Konan S, Tahmassebi J, Rowan F, Haddad F. An assessment of early functional rehabilitation and hospital discharge in conventional versus robotic-arm assisted unicompartmental knee arthroplasty: A PROSPECTIVE COHORT STUDY Bone Joint J 2019;101-B:24–33
- Kayani B, Konan S, Tahmassebi J, Pietrzak J, Haddad F. Robotic-arm assisted total knee arthroplasty is associated with improved early functional recovery and reduced time to hospital discharge compared with conventional jig-based total knee arthroplasty: A PROSPECTIVE COHORT STUDY Bone and Joint Journal: 2018; 100-B:930–7.
- Shibanuma N, Ishida K, Matsumoto T, et al. Early postoperative clinical recovery of robotic arm-assisted vs. image-based navigated Total hip Arthroplasty. BMC Musculoskelet Disord. 2021;22(1):314.
- Fontalis A, Kayani B, Asokan A, et al. Inflammatory Response in Robotic-Arm-Assisted Versus Conventional Jig-Based TKA and the Correlation with Early Functional Outcomes: Results of a Prospective Randomized Controlled Trial. J Bone Joint Surg Am. 2022;104(21):1905-1914. doi:10.2106/JBJS.22.00167
Hip & Knee Replacements
Hip joint replacement is intended for use in individuals with joint disease resulting from degenerative and rheumatoid arthritis, avascular necrosis, fracture of the neck of the femur or functional deformity of the hip.
Knee joint replacement is intended for use in individuals with joint disease resulting from degenerative, rheumatoid and post-traumatic arthritis, and for moderate deformity of the knee.
Joint replacement surgery is not appropriate for patients with certain types of infections, any mental or neuromuscular disorder which would create an unacceptable risk of prosthesis instability, prosthesis fixation failure or complications in postoperative care, compromised bone stock, skeletal immaturity, severe instability of the joint, or excessive body weight.
Like any surgery, joint replacement surgery has serious risks which include, but are not limited to, pain, infection, bone fracture, change in the treated leg length (hip), joint stiffness, hip joint fusion, amputation, peripheral neuropathies (nerve damage), circulatory compromise (including deep vein thrombosis (blood clots in the legs)), genitourinary disorders (including kidney failure), gastrointestinal disorders (including paralytic ileus (loss of intestinal digestive movement)), vascular disorders (including thrombus (blood clots), blood loss, or changes in blood pressure or heart rhythm), bronchopulmonary disorders (including emboli, stroke or pneumonia), heart attack, and death.
Implant related risks which may lead to a revision of the implant include dislocation, loosening, fracture, nerve damage, heterotopic bone formation (abnormal bone growth in tissue), wear of the implant, metal and/or foreign body sensitivity, soft tissue imbalance, osteolysis (localized progressive bone loss), audible sounds during motion, and reaction to particle debris. Hip and knee implants may not provide the same feel or performance characteristics experienced with a normal healthy joint.
The information presented is for educational purposes only. Speak to your doctor to decide if joint replacement surgery is appropriate for you. Individual results vary and not all patients will return to the same activity level. The lifetime of any joint replacement is limited and depends on several factors like patient weight and activity level. Your doctor will counsel you about strategies to potentially prolong the lifetime of the device, including avoiding high-impact activities, such as running, as well as maintaining a healthy weight. It is important to closely follow your doctor’s instructions regarding post-surgery activity, treatment and follow-up care. Ask your doctor if a joint replacement is right for you.
Stryker Corporation or its other divisions or other corporate affiliated entities own, use or have applied for the following trademarks or service marks: AccuStop, Mako, SmartRobotics, Stryker. All other trademarks are trademarks of their respected owners or holders.
JR-GSNPS-PTNT-729650